“Not a lot of people have an opportunity to make an unexpected discovery that leads to a dramatic program that really impacts the lives of millions and millions of people. But when you do, it is your responsibility to change clinical practice,” says Alfred Sommer, an ophthalmologist at John Hopkins University who lives by this principle.
Sommer earned the Albert Lasker Clinical Medical Research Award in 1997 for converting his discovery that vitamin A reduces mortality rates for common infections in children to national-level health programs in multiple countries. His saga is full of surprises, challenges, patience, and perseverance.

Sommer in his office in 2017
[Courtesy of Fred Dubs]
Sommer’s grandmother told him when he was very young that he would become a doctor — a prediction that remained deeply implanted in his mind. After fulfilling her prophecy by graduating from Harvard Medical School, Sommer landed an opportunity to work on an epidemiology project in what was then East Pakistan (now Bangladesh). During his time there, he saw numerous tragedies, including a cyclone that affected a quarter of a million people, war, and a smallpox outbreak. As he assisted with relief and rehabilitation projects, he realized that epidemiology was a powerful tool that could impact the health of large numbers of people. This prompted him to change his focus from internal medicine to epidemiology, followed by specializing in ophthalmology.
During his residency at Johns Hopkins University, Sommer took up an interesting collaborative project. Researchers had implicated vitamin A deficiency in xerophthalmia — childhood blindness — especially in developing countries where micronutrient deficiencies were common. Xerophthalmia manifests as night blindness in children, deteriorating further into complete blindness if left untreated. Many children in the developing world were vitamin A deficient, but not all of them suffered from blindness. Sommer was intrigued by these differences and started investigating the role of vitamin A in children’s health.
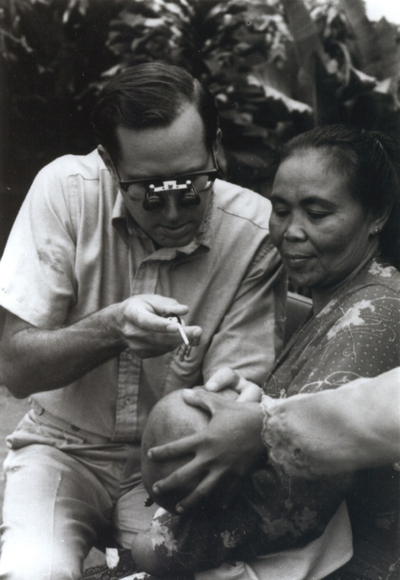
Sommer examining a child at the start of his vitamin A research in Indonesia (1976)
Leveraging his epidemiology and ophthalmology expertise, Sommer set up a number of field studies in Indonesia from 1976 to 1979 to compare the health of children who developed night blindness or other eye diseases versus that of those who did not develop any eye disease. For one study, he and his team followed the health of 4600 children in rural Indonesia over 18 months. They examined the children at the beginning of the trial and reexamined them at intervals of three months for six rounds. Little did he know that this study would change the lives of millions of people, including his own.
The Unexpected Connection
One Saturday afternoon just before Christmas in 1982, Sommer was analyzing data from this field study. While tracing the progress of children from the baseline exam to the follow-up checkups, he noticed an unanticipated trend. Children with night blindness at one exam were less likely to appear for their follow-up exam three months later. By digging further into the records, he realized the reason for their absence: they were dying.
Sommer wondered if there was a link between blindness and death. He tasked a newly hired statistician, Joanne Katz (now the director of academic programs at Johns Hopkins Bloomberg School of Public Health), with her first project. Katz reanalyzed the data from a different perspective to answer the question: does eye disease from vitamin A deficiency increase the risk of death within three months?
The answer was yes. Children with vitamin A deficiency were not just prone to blindness but were also dying at a higher rate than children who had healthy eyes and a slightly better vitamin A status three months earlier. The team also noted a dose-response relationship, meaning that children with mild vitamin A deficiency were three times more likely to die than those without deficiency, and those with severe deficiencies were nine times more likely to die.
Sommer was overwhelmed.
“This is unbelievable; looks like two cents’ worth of vitamin A could reduce child mortality by a third!”
Excited, the team published their findings in the medical journal The Lancet. There was just one problem. “Absolutely nobody believed it! The idea that mild vitamin A deficiency might be an important cause of child mortality seemed totally beyond anybody’s ability to comprehend,” recalls Sommer.

Researchers who analyzed data from the first randomized trial assessing the impact of vitamin A supplementation on child mortality in Aceh, Indonesia (1986)
Overcoming All Hurdles
Undeterred, Sommer’s team set out to collect further evidence. Over the next few years, he and Katz designed several randomized trials to ensure that vitamin A deficiency was the key factor increasing the risk for child mortality.
These were large-scale studies involving 20,000 children across 500 villages in developing countries. For every trial, half of those in a study were given vitamin A capsules and the other half were given a placebo. In this way, the only difference between the two groups was one factor: vitamin A status.
Upon publication of the studies, the team again met with skepticism from their colleagues. “Not only did they not believe the initial results, they said we didn’t know how to do studies, and we had done them wrong,” says Sommer.
But criticism did not deter Katz. “I took it as a challenge; if people wanted more data to be convinced, it was a good thing,” she says.
More and more data poured in, supporting their initial results. Vitamin A supplements reduced child mortality rates by a third. To Sommer, it seemed clear that vitamin A deficient children had a very poor immune response to common illnesses. Whereas all children were exposed to the same infectious diseases, primarily diarrheal diseases and measles, those who were vitamin A deficient could not fight off the infection as well as those who had normal vitamin A levels.
By 1992, after multiple studies showing similar results and collecting other corroborating evidence, Sommer had had enough. “It was unethical to do any more of these studies,” Sommer recalls.
“There was so much evidence, at least as far as I was concerned, that I couldn’t do any more of these studies.”
He decided to put an end to the debate once and for all. He called a meeting of experts for a conference at the Rockefeller Center in Bellagio, Italy, and presented the collective data and facts. At the end of the conference, he asked everyone to sign a statement of agreement announcing that there should not be any more randomized trials for vitamin A.
The unanimous acceptance of the results produced the desired effect. Leading medical experts across the world submitted conclusions from the meeting to medical journals, and the wheels turned. Within a few months, the World Health Organization and UNICEF launched a global vitamin A deficiency prevention program, providing about half a billion vitamin A supplements to over 50 countries every year and preventing death and blindness in about 250,000 children every year.
It took him almost a decade, but through his dedicated efforts, Sommer finally convinced the world of the importance of vitamin A for public health. A lot has already been accomplished on this front, but the work continues, says Sommer. For instance, what remains is to find a simple way of administering vitamin A. The current system in most countries involves local volunteers providing each child with a large dose of vitamin A (200,000 units) twice a year. For a few countries, such as India, that are against the ‘magic capsule’, developing low-cost fortified foods would help, according to Katz.

In 1986, Hugh Downs and his team from 20/20 decided to cover Sommer’s vitamin A research trial in the Philippines. “I vividly recall him calling me at Hopkins to say they were planning to do this the following week and expected me to be there,” Sommers recalled. “I told them I knew nothing about it, and had a long list of surgical procedures scheduled that week. He replied, ‘If you don’t go, we don’t go.’ I went.”
The Power of Perseverance
A stroke of luck to stumble onto something significant and the scientific acumen to realize its importance are certainly prerequisites for this success story, but the power of perseverance was key. The initial discovery is just the first step in most cases. Follow-up often determines the fate of the discovery — whether it will reach the clinic or remain as a note in a lab book.
Sommer’s data-driven approach and perseverance kept him and his team going in tough times. “We will just keep doing these studies until they are so buried in data, they have to accept it,” Sommer once told his young recruits when they were disappointed about the negative comments from peers.
“You don’t convince the world by screaming and yelling and having debates. You convince the world by replicating the studies and showing again and again that the observations are, in fact, true.”
It took nine years of struggle for Sommer to convince his peers and bring about change at a global level, but the effort saved millions of lives. “If you make a discovery that has clinical relevance that can have a major impact on people’s lives, you have an ethical responsibility to see that to fruition,” he says.
By Meenakshi Prabhune
